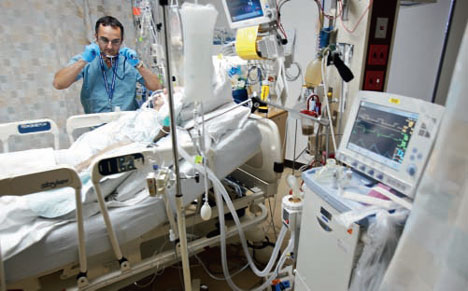
When people hear about those who suffer from Post Traumatic Stress Disorder (PTSD), they might think about soldiers who fought in a war or victims of heinous violence, but a lesser known group of sufferers have been making headlines recently: Intensive Care Unit patients.
These patients are typically fighting a critical illness and go into the ICU fighting for their lives, but come out suffering from hallucinations, nightmares and memory loss.
PTSD can also make it difficult to connect with others and experience joy.
In 2013, Texan registered nurse Lygia Dunsworth told the New York Times about her horrific account of what it was like to suffer with PTSD as a patient.
Dunsworth was critically ill due to abdominal infections and surgeries, and she wound up sedated, intubated and strapped down while receiving care in an ICU at Fort Worth hospital.
She was dismissed after her treatment, but her time in the ICU haunted her for years to come.
She suffered from the following hallucinations:
-
helicopters evacuating patients from an impending tornado
-
Nurses plotting to toss her into rough lake waters
-
Ducking into a food freezer, surrounded by body parts during an attempted escape from the ICU
She never wanted to talk about her experience for fear of sounding crazy, but she suffered from short term memory loss, difficulty sleeping, fear of bodies of water and fear of traveling alone--all related to PTSD, and her experience isn’t all that unique.
In early 2015, a Johns Hopkins research team analyzed over 40 studies involving more than 3,000 patients who spent time in the ICU while critically ill (but excluded patients who had suffered physical traumas like car crashes or brain injury).
From this group, the researchers whittled down to a subset of six studies and 450 patients who were being assessed with a PTSD measurement tool called the Impact of Event Scale once they left the ICU.
One in four patients who left the ICU between one to six months ago were found to have PTSD, and 1 in 5 patients who left between seven to 12 months ago continued to suffer from PTSD.
"These rates are as high as you might see in combat soldiers or rape victims," Dale Needham, M.D. told Science Daily.
For years, Dr. Needham, a professor of medicine and of physical medicine and rehabilitation at Johns Hopkins, has studied what happens to patients after they leave ICU.
"We analyzed the physical, cognitive and psychological effects of their critical illness/ICU care and uncovered an array of challenges that are clinically referred to as post-intensive care syndrome."
When it comes to identifying patients who are most susceptible research found people who were previously diagnosed with a psychological condition, such as anxiety or depression, or patients who received a lot of sedation medication during their time in the ICU had higher incidents of PTSD.
Needham said patients who return home mentally shaken or with physical and cognitive weaknesses may remain that way up to two years after treatment, which can place a lingering burden on both the patient and the family.
Thankfully, a powerful, yet deceptively simple method is being used to help prevent ICU related PTSD, an ICU diary. The diary serves as a notebook that family members, nurses and other clinicians can write in daily to document patient treatments and events related to the patient.
ICU diaries are relatively new to the United States, but are commonly used in Europe.
The New York Time reports that nurses and family members in Britain, Germany and some Scandinavian countries, also keep a diary that they give to the patient once they leave.
Joe Bienvenu, M.D., associate professor of psychiatry and behavioral sciences at the Johns Hopkins University School of Medicine believes diaries help patients recall their experiences more accurately.
“They provide patients with a tool to better understand their experience in the ICU through the words of their loved ones and caregivers," he said.
Each year, an estimated 5 million people end up needing ICU level care and more than 750,000 end up needing ventilators. With a growing number of ICU “survivors” making it through critical care and life saving treatments, Needham says clinicians and patients alike need to be aware of the PTSD risks that exist for patients who survive major illnesses.
To learn more, see Science Daily’s Report here: http://www.sciencedaily.com/releases/2015/04/150420144753.htm
New York Time’s report here:
http://well.blogs.nytimes.com/2013/07/22/nightmares-after-the-i-c-u/?_r=1