Posted by Zunaira Rizwan, MBBS
Nurses play a significant role in caring for patients with stroke. By recognizing early signs of decline, nurses take the first step toward preventing a stroke patient from deteriorating. While many stroke patients are stabilized after an acute phase, deterioration can occur at any time. Being aware of the clinical signs of neurological decline helps spot them early, thereby preventing drastic sequelae of a stroke. In this blog, we will discuss these signs and how to notice them before it's too late.
Why Early Recognition Matters
A stroke is a medical emergency that can continue to worsen beyond the acute phase. A variety of causes can contribute to the neurological decline, including cerebral edema, hemorrhagic transformation of stroke, seizures, metabolic disturbances, or a new vascular event. After a stroke, the brain is highly sensitive to these changes, and without prompt intervention, permanent damage can ensue.
Therefore, you must be aware of the signs of deteri...
Posted by Nicole Ricketts-Murray, RN
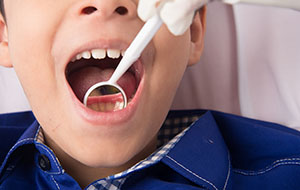
Oral health is a foundational yet sometimes underestimated component of pediatric preventive care. For children, the mouth is not an isolated system; it is intricately connected to nutrition, speech development, growth, and systemic health. Increasing evidence from reputable organizations such as the Centers for Disease Control and Prevention (CDC), the American Academy of Pediatric Dentistry (AAPD), and the American Heart Association (AHA) reinforces the importance of maintaining good oral hygiene in childhood, with implications far beyond preventing tooth decay. Routine habits like brushing and flossing teeth are central to preventive dental care, reducing the risk of childhood cavities and contributing to overall health outcomes across the lifespan.
The Burden of Pediatric Oral Disease
Dental caries remains the most common chronic disease of childhood. According to the CDC, approximately one in five children aged 5 to 11 years has at least one untreated decayed tooth, and ...
Posted by Nicole Ricketts-Murray, RN
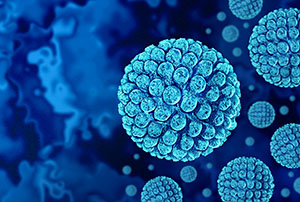
Each winter, public health officials in New York and across the United States brace for a predictable yet persistent foe: norovirus — the highly contagious virus responsible for most acute gastroenteritis outbreaks. Often dubbed the “winter vomiting bug,” norovirus consistently peaks in colder months, exploiting close-contact environments such as schools, childcare settings, and long-term care facilities where transmission spreads rapidly.
For healthcare providers, infection prevention specialists, and facility administrators in New York, understanding the epidemiology, transmission dynamics, and evidence-based mitigation strategies of norovirus is essential to safeguarding vulnerable populations and reducing outbreak impacts.
What is Norovirus?
Norovirus is a group of highly contagious viruses that cause acute gastroenteritis — inflammation of the stomach and intestines resulting in vomiting, diarrhea, nausea, and abdominal cramps. Symptoms m...
Posted by Nicole Ricketts-Murray, RN
For anyone working as a nurse, physician assistant, pharmacist, social worker, or in any other licensed healthcare role in New York, staying up to date on the state’s continuing education (CE) requirements is a central part of maintaining your professional license and your reputation. The rules can seem complex, thanks to the different mandates, changing regulations, and timelines unique to each profession. It’s perfectly normal to feel a bit lost or even overwhelmed by the process at times. That’s exactly why this guide exists: to clearly explain the most important CE rules for New York healthcare professionals. Here, you’ll find straightforward information tailored to your role, along with practical advice to help you remain compliant, renew your license on time, and deliver the highest standards of care without unnecessary stress.
Why Continuing Education Matters
Continuing education isn’t just another item to check off your to-do list—it&rs...
Posted by Nicole Ricketts-Murray, RN
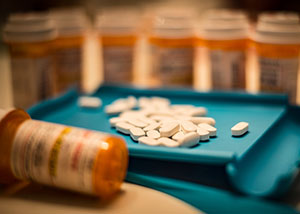
If you’re prescribing in New York, whether you’re a physician, physician assistant (PA), resident, or anyone else with a Drug Enforcement Administration (DEA) number, responsible prescribing isn’t just a box to check; it’s a professional and ethical responsibility. With the opioid crisis still looming large and state regulations getting stricter, knowing and following New York’s controlled substance rules is crucial to protecting both your patients and your own career.
This guide is here to help, highlighting the key laws, practical steps, and continuing education you’ll need for compliant, thoughtful prescribing in New York. You’ll find the latest on monitoring prescriptions, documenting your rationale, and more, so you can practice safely and confidently.
Why Responsible Prescribing Matters
When controlled substances, especially opioids, aren’t prescribed thoughtfully, the results can be tragic: lives lost to overdose, fami...