Category - infectious-disease
Posted by Nicole Ricketts-Murray, RN
Each winter, public health officials in New York and across the United States brace for a predictable yet persistent foe: norovirus — the highly contagious virus responsible for most acute gastroenteritis outbreaks. Often dubbed the “winter vomiting bug,” norovirus consistently peaks in colder months, exploiting close-contact environments such as schools, childcare settings, and long-term care facilities where transmission spreads rapidly.
For healthcare providers, infection prevention specialists, and facility administrators in New York, understanding the epidemiology, transmission dynamics, and evidence-based mitigation strategies of norovirus is essential to safeguarding vulnerable populations and reducing outbreak impacts.
What is Norovirus?
Norovirus is a group of highly contagious viruses that cause acute gastroenteritis — inflammation of the stomach and intestines resulting in vomiting, diarrhea, nausea, and abdominal cramps. Symptoms m...
Posted by Nicole Ricketts-Murray, RN
Infection control isn’t just a box to tick on a lengthy list of professional requirements—it’s truly at the heart of what it means to provide safe, ethical healthcare. Here in New York, the state has recognized this by requiring all licensed healthcare professionals to complete rigorous infection control training since August 1992, with important updates rolled out in 2008 and ongoing changes that now include sepsis education.
The expectation is simple but crucial: every provider must renew their infection control training every four years. This isn’t done just for a show; it’s a serious matter. Failing to stay current isn’t just a minor oversight—it’s considered professional misconduct and can put your license at risk in the eyes of state regulators.
The following guide is designed specifically for New York’s diverse healthcare community—nurses, doctors, dentists, optometrists, physician assistants, and allied healt...
Posted by Mary Thompson
Mpox, formerly known as monkeypox, is a zoonotic viral infection caused by the monkeypox virus, a member of the Orthopoxvirus genus, which is part of the same family as smallpox. While historically rare and largely confined to regions in Central and West Africa, Mpox has reemerged as a global public health concern in recent years, prompting renewed focus from healthcare systems around the world.
The 2022-2023 outbreak saw widespread transmission in countries where Mpox had never been endemic, including the United States, with New York City becoming a major epicenter. In response, the Centers for Disease Control and Prevention (CDC) and the World Health Organization (WHO) have continued to monitor cases, issue guidance, and recommend vaccination for high-risk populations. As we move through 2024 and 2025, Mpox remains a relevant and evolving concern.
This blog will cover everything New York healthcare professionals need to know about Mpox, including:
What it is and how it pr...
Posted by Dr. Julia Tortorice
Every day, people navigate a world dealing with invisible threats – germs lurking in unexpected places, just waiting to make them sick. These germ-laden areas pose potential risks to their health. Awareness and proactive hygiene practices are essential for mitigating these risks. Surprisingly commonplace items like kitchen sponges can collect more bacteria than expected, emphasizing the importance of understanding and addressing germ hotspots in everyday environments such as:
Public Transportation
Public transportation systems, such as buses, trains, and subways, serve as bustling hubs of activity where germs can quickly multiply due to the proximity of passengers and high traffic.
Hotspots: Handrails, seat handles, ticket machines, and other frequently touched surfaces within public transit vehicles are prime breeding grounds for germs, accumulating microbes from numerous individuals.
Safety Tips: To minimize the risk of germ transmission, individuals should utiliz...
Posted by Dr. Julia Tortorice
In the realm of healthcare, the battle against infectious diseases extends far beyond the physical ailments they inflict. As we navigate through the complexities of diseases that can spread with alarming rapidity, we confront not only the tangible impact on the body but also the profound psychological toll on both those diagnosed and the dedicated professionals who care for them. The psychological ramifications—ranging from heightened stress and anxiety to severe burnout and post-traumatic stress disorder (PTSD)—cast long shadows over the well-being of patients and healthcare workers alike.
For patients, the journey following an infectious disease diagnosis is often filled with fear, uncertainty, and isolation. The moment of diagnosis marks the beginning of a challenging path, where worries about health outcomes, potential stigma, and the strain of treatment protocols can lead to profound emotional distress. The isolation required to prevent disease transmission, while m...
Posted by Julia Tortorice
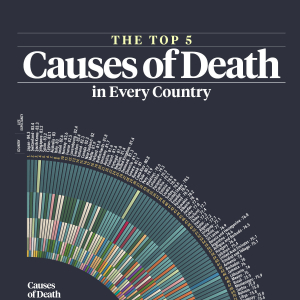
Death may be inevitable, but there are plenty of efforts we can make to help us enjoy longer, healthier lives. By understanding the health risks that are the most prevalent in our communities, we can be more proactive on a personal level and empower others to do so as well. To help with that goal, the team at NYRequirements.com has created this visual guide to the leading causes of death by country and average life expectancy by country. As the most common cause of death by country is often heart disease, we also delve more into the causes of heart disease and how to reduce heart disease risk below. For now, let’s learn about the biggest causes of death globally:
Click here to view PDF mobile version of the chart.
What Is the Leading Cause of Death in the World?
The leading cause of death globally is cardiovascular disease.
How Many People Die From Heart Disease Each Year?
Cardiovascular diseases cause an estimated 17.9 million deaths per year, most often (4 out of...
Posted by Julia Tortorice
After years of being in the grip of a global health emergency, the light at the end of the tunnel is finally visible. With the recent declaration to end the federal public health emergency (PHE) in the United States, we officially live in a post-COVID-19 emergency world. Or do we? As restrictions continue to ease, there is, undoubtedly, a sigh of relief sweeping across the country. However, the pandemic has left a profound mark on society.
The effects of the COVID-19 pandemic can especially be felt in the healthcare industry, where a period of unprecedented challenges, losses, and continuous adaptation has happened and continues to occur on a regular basis. Now that the PHE has come to an end, what can we expect to happen? It’s time to explore what lies ahead and how to navigate what is headed our way.
What to Expect
While the situation may vary from region to region, most of the post-emergency expectations are fairly general to everyone across the board as we move forwa...
Posted by Julia Tortorice
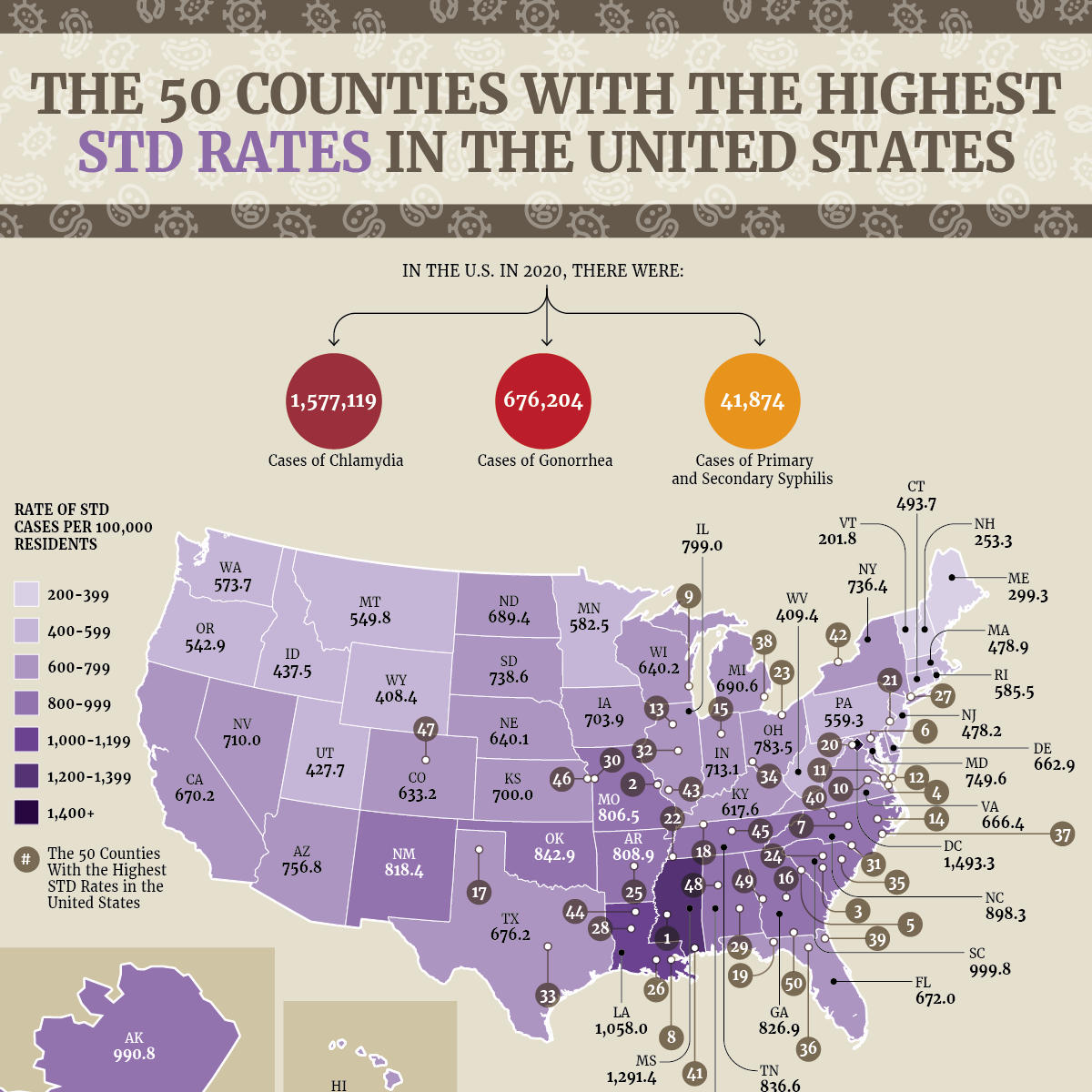
The number of STD cases in the United States has been surging over the past few years, with more than 2 million cases of chlamydia, gonorrhea, and syphilis diagnosed in 2020. According to the CDC, STD rates have reached an all-time high and the progress the agency had made to control the spread of STDs has “unraveled.” Less than 20 years ago, the number of new STD cases was far lower, with chlamydia being easier to detect, gonorrhea rates at historic lows, and syphilis close to being eliminated.
The team at NYRequirements.com wanted to know if certain areas of the country were being hit harder by this uptick in common STDs. Using county data collected through the CDC’s NCHHSTP AtlasPlus, our team analyzed the rates of the most common STDs in the U.S. to determine the 50 counties with the highest rate of all STDs per 100,000 residents. Only counties with 100,000 residents or more were included in this analysis. The list of STDs includes chlamydia, gonorrhea, a...
Posted by Julia Tortorice
Which viruses in history were the fastest to spread throughout society? The NY Requirements team compared the basic reproduction number (R0) of 26 different viruses that require human-to-human transmission to see which were found to spread to the most people during the height of the virus outbreak. The basic reproduction number is a range of the number of people that one person will likely infect with the virus, a commonly used unit to compare the transmission rate of diseases. These infectious viruses can be spread through various methods of transmission, such as respiratory droplets, airborne, fecal-oral, or body fluids.
In addition to the basic reproduction number of these virus superspreaders, our team also found the number of new cases of each virus, whether it was during a major outbreak or the number of new cases that are contracted annually. We also examined the transmission method of the virus and whether or not a vaccine for the virus is available. Continue reading t...
Posted by Emily Pazel
Although there has been a lot of information gathered and shared about humans passing diseases and viruses around, you don’t often hear about animals spreading them. Because we can’t directly communicate with animals, it’s hard to know what is harming them or even when they are sick. However, it does happen – probably more often than you think. There are instances where diseases are spread from animal to animal and then also from animal to human and vice versa.
So, how does this work exactly? Pets can be very beneficial to humans on many levels, both physically and mentally. It’s more common than ever these days to see a home with one or more pets in it, and it’s good to know what to look for if your pet may be showing symptoms of carrying a virus or if it’s possible to spread the virus to them.
How to Tell If Your Dog is Sick
Although your dog can technically get sick, according to wagwalking.com, it’s fairly rare to give your d...
Posted by Julia Tortorice
Click here to download the printable PDF version of the chart
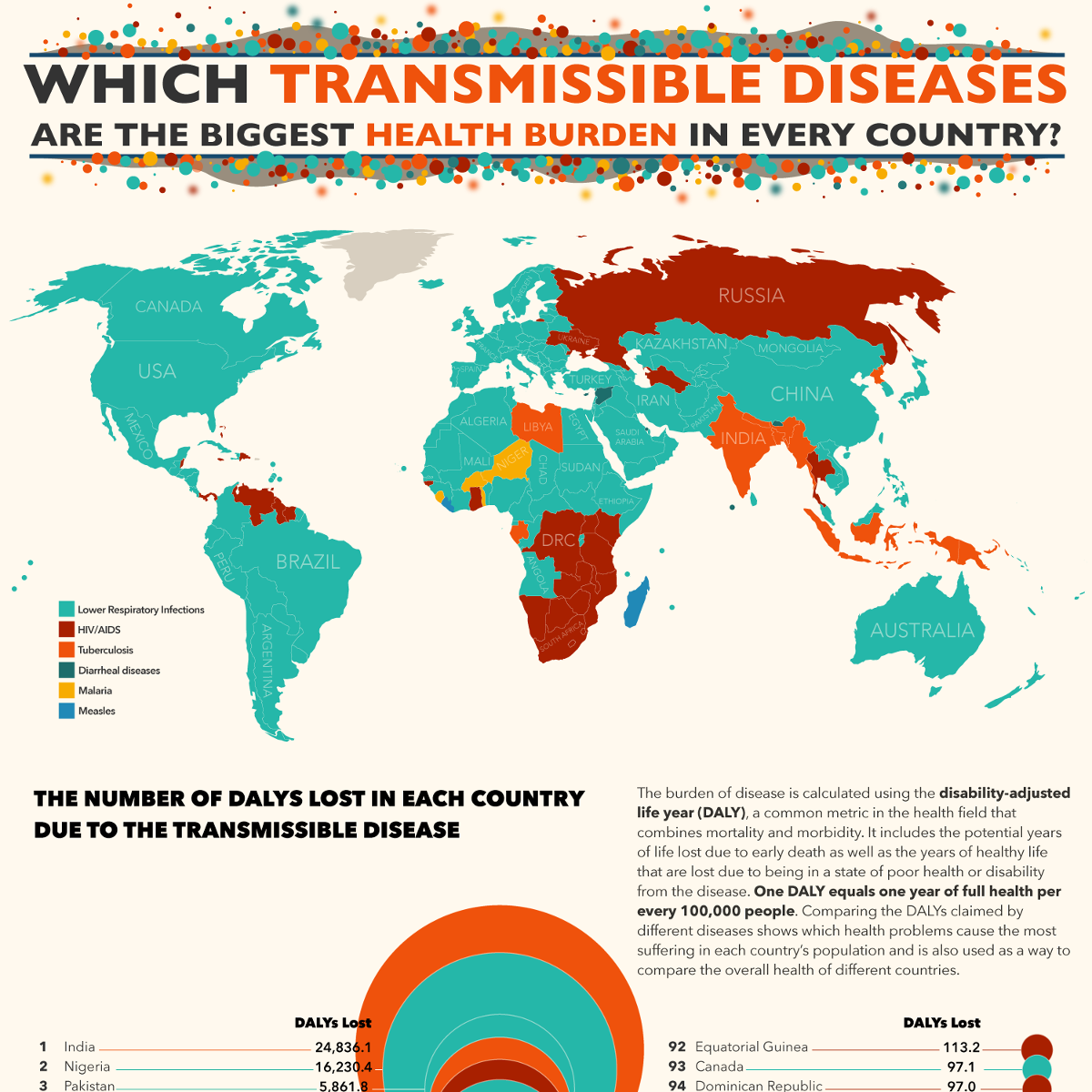
A wide variety of transmissible diseases are passed from one person to another within countries and around the world, but which of these contagious diseases is the biggest health burden in each country? Using burden of disease estimates from the World Heath Organization's (WHO) Global Health Estimates (GHE), we analyzed 40 different communicable diseases to see which types of disease caused the highest loss of daily adjusted life years (DALYs) in each of the countries around the world. DALYs are a common health metric because they combine the burden of mortality and morbidity to determine the sum of years of healthy life that are lost due to the disease in a country’s population.
The NYRequirements.com team analyzed a wide variety of infectious, parasitic, and respiratory diseases, including HIV/AIDS, STDs, childhood-cluster diseases, hepatitis, intestinal nematode infections, as well as disea...
Posted by Emily Pazel
We all get sick from time to time – it’s nature’s way of helping us build up our natural immunity so that we can defend ourselves against disease-causing microorganisms. However, getting sick during this process is never fun for anyone, especially when you already have a fairly busy, stressful schedule. So, the bigger question is: Is there a better way to help build your immune system naturally?
Fortunately, there are different ways to help boost your immune system naturally by adding vitamins and supplements into your diet and making other lifestyle changes to help swing your health into a more positive direction. But before we dive into how to achieve this goal, let’s first talk about the immune system and the role it plays in helping your overall health.
The Immune System 101
Learning about the immune system is hopefully something you learned early on in school when learning how your body fights off germs. However, there’s definitely no time li...
Posted by Julia Tortorice
Click here to download the printable PDF version of the chart
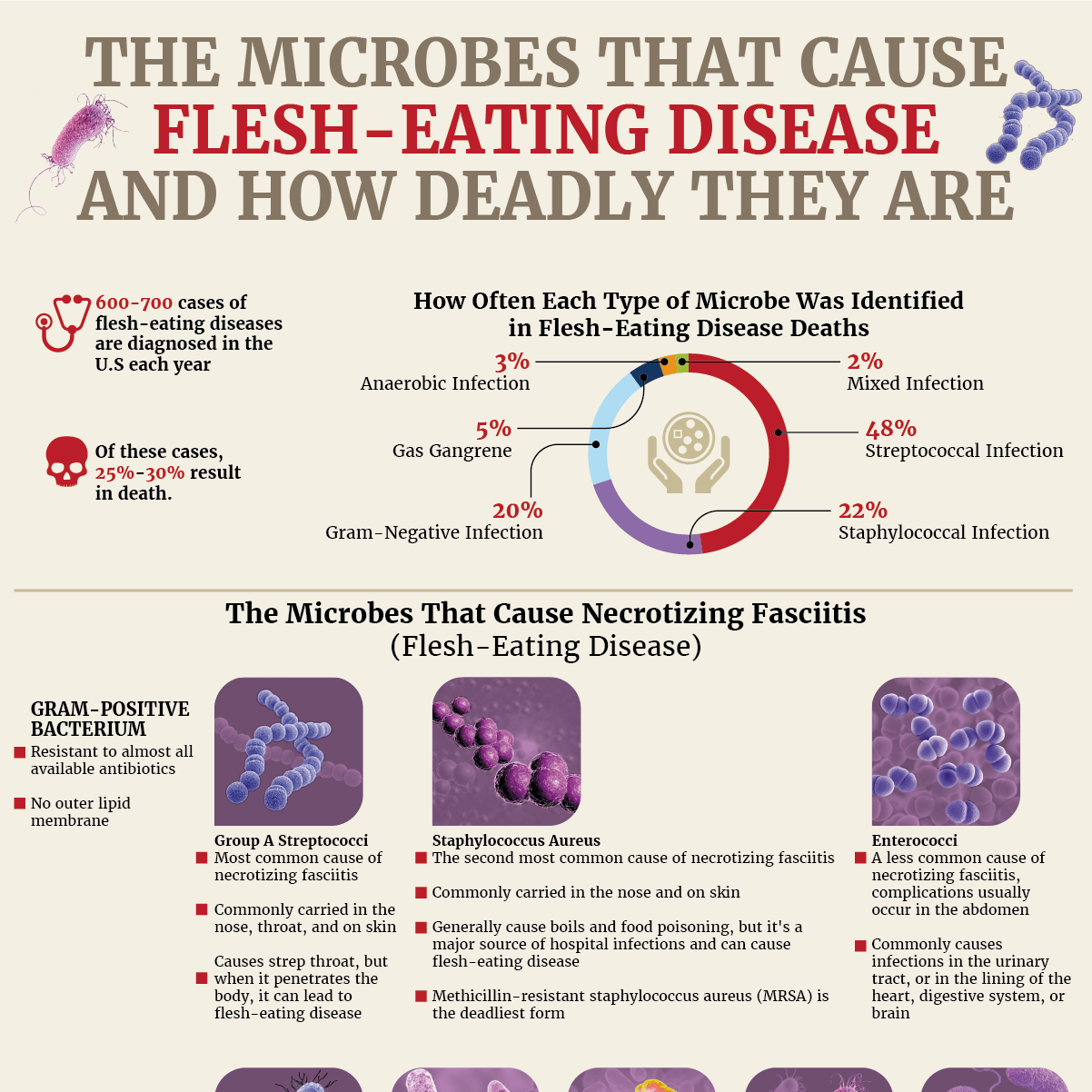
Flesh-eating disease: Just the name alone is enough to send shivers down your spine. But what causes it to develop, and how often are people diagnosed with this horrific condition? You may be surprised to learn that the flesh-eating bacterium that is known to cause necrosis or gas gangrene may be on your skin or in your nose at this very moment. It turns out that the strep bacterium that causes an annoying and painful strep throat is the same microbe that is responsible for causing the most cases of flesh-eating disease.
Read on to see which types of skin-eating bacteria, as well as a certain type of fungus, are responsible for the hundreds of cases of necrotizing fasciitis that occur each year in this infographic from NYRequirements.com.
What Is Flesh-Eating Disease
Flesh-eating disease, also known as necrotizing fasciitis, is a rare bacterial skin infection that can spread quickly throughout...
Posted by Emily Pazel
Even though the flu isn’t new and is even fairly common around this time of the year, something strange is happening this season. For the past few years, people have been quarantining, social distancing and helping slow the spread of germs and viruses around the world. However, as national mandates slow down and people start to return to their normal lives, people are starting to come down with the flu and the coronavirus, and in some cases – maybe both at the same time?
As more cases have come forward recently, it does seem that you can have the flu and the coronavirus simultaneously. In fact, there have been some, but very rare, cases where an individual has tested positive for COVID-19 and then tested positive for influenza within days of each other. Although they are similar and can have similar symptoms, they are different and humans are able to catch a strain of each, sometimes even days or maybe hours apart.
By breaking down the science behind both viruses and ...
Posted by Emily Pazel
When the most recent pandemic began, roughly two years ago, it came as a pretty big shock to some as the world began to change. It seemed as though a Hollywood movie had become reality as the world was asked to change their way of life to get through a global pandemic. Many were asked to stay home, others were deemed “essential workers” and continued to work in person. Most classrooms and schools became a virtual learning center, and everyone was asked to “socially distance”, in an attempt to help slow the spread of the virus.
If you fast forward a few years to the present time, things are better than they were during the height of the pandemic, but we are not fully back to how things used to be. And, it’s believed that things may never get back to normal for a while, especially if you work in the healthcare industry where masks and other precautions are most likely to become the new norm. As things get back to normal, however, it’s interesting t...
Posted by Emily Pazel
If you are like the millions of Americans who felt like this past year has been anything but ordinary, you will be glad to know that things are starting to head back to normal life. Or, at least as normal as things can be during a global pandemic. Especially in the state of New York, businesses, schools and other in-person activities have started to return back as we head into a nearly post-pandemic world.
“Most businesses and schools are now allowed to be open in New York City,” writes NYC Health. “Employers, administrators and other responsible parties must review, attest to and comply with New York State’s industry-specific guidance.”
For several months, New York and the surrounding areas were hot spots for COVID-19 and the city was ultimately on lock down to help slow the spread of the virus. With many of the state becoming vaccinated and infection rates at the lowest the state has ever seen, the state has started to slowly lift restrictions on i...
Posted by Emily Pazel
When the Coronavirus first made its way across the United States near the beginning of 2020, New York City and the surrounding areas were one of the hardest-hit places with positive cases and deaths. Now, with the holiday season in full swing, the governor announced near the middle of December that there were a new record high number of COVID-19 tests reported.
Although the vaccine has made tremendous leaps and bounds on being created and released quickly, it still may take awhile before everyone is properly vaccinated. And with that, some holiday traditions – such as the iconic New Year’s Eve Ball Drop in New York City’s Times Square – will have to take place virtually. Back in September, event organizers released a video and announcement saying the holiday event would happen “visually, virtually and safely.” The organizers also included that they would make sure anyone could tune in to easily watch it. Not only will major news networks carry liv...
Posted by Emily Pazel
As if the pandemic couldn’t get any worse, a recent study published in Science confirms that a new strain of the coronavirus has mutated and its mutation has enabled it to spread more quickly around the world. The good news, however, is that the mutation may also make the virus more susceptible to a vaccine.
The new strain of the coronavirus, known as D614G, is different from the original strain that came from China at the beginning of the pandemic. Research from the University of North Carolina at Chapel Hill and the University of Wisconsin-Madison show that the newest strain replicates at a faster rate and is more transmissible. Studies have also shown that even though this particular strain spreads faster, it is not associated with a more severe disease and is more sensitive to antibodies used in vaccines.
The study of this recent mutation was published around the middle of November, and provides some of the first real, concrete findings about how the virus is stea...
Posted by Emily Pazel
You might think that something as scary as a brain-eating amoeba could only be found in a science fiction movie, but it’s not – it’s actually a real thing. So real in fact, that it’s recently stirred up some news around the country. In Florida, a 13-year-old boy was hospitalized and ultimately died after vacation in a freshwater source around North Florida. And several cities in Texas were issued an emergency alert after a young boy was hospitalized after playing in a public fountain and using a hose in his front yard.
While this sounds like something that could keep you awake all night or leave you with never wanting to swim in a lake again, you’ll be glad to know that these situations are typically very rare. But it does raise some questions, such as what are my chances of contracting this infection? How severe can the infection become? Are there ways to prevent it?
Unfortunately, not much is known about this brain-eating amoeba other than it exist...
Posted by Emily Pazel
How to Become a Disease Expert
With a global pandemic sweeping the streets, scientists and medical professionals have teamed up together to create and implement safe guidelines for people to take steps to help slow the spread of the Coronavirus. If you have a social media page or listen to the news, you might have noticed that one of the world’s top leading scientists helping implement these strategies in the United States, Dr. Anthony Fauci, has a background in infectious diseases, which is a specialization in public health sciences.
So, what makes him qualified enough to help lead the nation through a global pandemic? Have you ever considered going into the field of epidemiology? Although a global pandemic might not be a common occurrence, we may find a rise in students interested in choosing a career path in this field, or more people learning about it to help keep their business open during a time where a virus is easily spreading person to person.
What is Epidemiolo...
Posted by Emily Pazel
As the spread of the global pandemic continued to touch cities and hometowns all over the United States, busy streets went empty, restaurants went dark and the normal hustle and bustle of thriving cities, such as New York City, declined in a way that we never saw coming. If you live in the state of New York or anywhere near the city, you might have witnessed several changes in your town, including the collapse in the tourism industry, leaving thousands without jobs and many businesses, theaters, sightseeing tours, mass transportation services and other establishments hurting for prosperity and going back to a normal life.
With a hurting economy and social distancing guidelines established for safety precautions making it tough to get back to any kind of “normal” life, how does this affect the future of the industry going forward? Is there any hope of seeing large crowds gathering for a parade or celebration? What about all the daily sightseeing tours that bring in hundre...
Posted by Emily Pazel
Were you ever worried as a young child that your classmate had “cooties” and he or she could pass them onto you by giving you a hug or touching your hand? Although “cooties” is a made-up, fictitious way of describing imaginary childhood germs, it’s a concept that we learn as young children about keeping our hands to ourselves to slow the spread of germs around us.
Unfortunately, for all the germaphobes out there, germs are everywhere. And when we say everywhere, that’s exactly what we mean – they are in the air, on food, plants and animals, in the soil and water and just about every surface, including your own body. The good news, however, is that most germs can’t harm you because your immune system does a great job of fighting them off and protecting you against most infectious agents. However, there are some occurrences where germs can get tricky and mutate into something your body can’t handle, which can cause you to get sick....
Posted by Emily Pazel
It’s that time of year again when people walk around sneezing and spreading their germs all over the place, unintentionally. And sometimes, those germs contain powerful strains of a flu virus, which if left unprotected, can be deadly. In fact, the Center for Disease Control and Prevention (CDC) has released a recent report showing that at least 1,300 people have died from the flu so far this season.
Another key point that the CDC has released regarding this flu season is that type of flu strain that’s spreading is the influenza B/Victoria virus, which is unusual for this time of the year. Typically, the specific type of virus making its way around the streets isn’t the usual culprit for this time of the year, which adds a surprising element.
The Current Flu Season
So far this season, the CDC reports that there have been at least 2.6 million flu illnesses and 23,000 flu-related hospitalizations. Which unfortunately, scientists are saying could be a...
Posted by Emily Pazel
Your teeth are unique to you. So unique, in fact, that no two people’s teeth are the same – even for identical twins. For years, detectives have been able to use dental records to occasionally identify human remains due to this fact.
An important part of being an adult and maintaining a healthy lifestyle is taking care of your pearly whites. After all, once you lose your baby teeth, you only have one set of permanent teeth to last an entire lifetime, so it’s important to keep them as healthy as possible. Plus, who actually likes getting their teeth drilled into for cavities and other procedures? It’s better to just nip it in the bud and take care of your teeth on a daily basis, the right way.
National Dental Hygiene Month is celebrated in October, which means that before you get too deep into all the candy corn and pumpkin spice lattes, remember that taking care of your teeth is essential to maintaining a healthy lifestyle. Let’s start by...
Posted by Emily Pazel
Humans aren’t the only ones enjoying the long, hot summer days. Around this time of the year, mosquitoes are in full bloom – breeding, flying around and spreading deadly diseases around the world.
Although mosquitoes are relatively small insects, they are one of the most deadliest animals on the plant, according to the World Health Organization (WHO). Every year, they carry and manage to spread diseases to humans, causing millions of deaths around the world. In 2015, WHO stated that an estimated 438,000 people died from malaria alone, and that more life-threatening diseases such as Zika, West Nile virus, yellow fever, dengue, and others, are making their way across the world with a little help from the mosquito – no doubt.
By now, if you’re like me, you might start to feel your skin crawl just thinking about mosquitoes. Maybe even feel a little more… itchy? But don’t worry – we’re not just here to talk about all the dea...
Posted by Emily Pazel
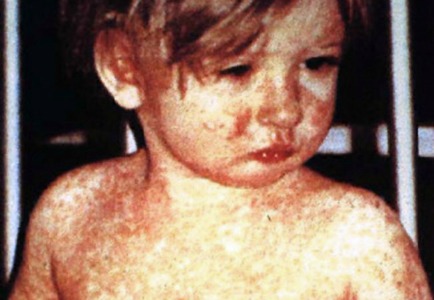
The measles outbreak happening in the United States has seen the highest number of cases reported since 1994, according to the Centers for Disease Control & Prevention (CDC). Since the beginning of this year, over 700 individual cases throughout 22 different states have been confirmed through the CDC.
Although measles was declared eliminated in 2000, the contagious disease has made its way back into the system and has been reported in Arizona, California, Colorado, Connecticut, Florida, Georgia, Illinois, Indiana, Iowa, Kentucky, Maryland, Massachusetts, Michigan, Missouri, Nevada, New Hampshire, New Jersey, New York, Oregon, Texas, Tennessee, and Washington.
So, how did it return? According to the CDC, it could have been brought to the country from travelers who contracted the disease abroad and it could be further spread within communities where people remain unvaccinated. Therefore, it is important to understand the signs and symptoms associated to measles.
Know the Sig...
Posted by Sandy Thompson
What is it :
Candida auris (C. auris) is a species of fungus that grows as yeast. It causes serious infections and is the leading cause of candidemia (candida infection of the bloodstream). C. auris is multidrug-resistant and has caused serious outbreaks in several countries. Due to its difficulty to identify and treat, C. auris has quickly become one of 2019 most concerning infectious diseases and presents a serious global health threat.
Where did it come from:
C. auris was first described as a pathogen in 2009 in Japan, when it was isolated from a patient with an ear infection. Retrospective review of Candida strain collections found that the earliest known strain of C. auris dates to 1996 in South Korea. The CDC considers C. auris an “emerging pathogen” because increasing numbers of infections have been identified in multiple countries since it was recognized.
Why is it concerning:
The C. auris fungus causes invasive infections with a high death rate...
Posted by Sandy Thompson
Over the last year, talk about a possible smallpox re-emergence has been spreading. We will take a deeper look into this historic disease and try to determine why there is a growing concern, how can it affect us all and what can we do to protect ourselves?
“Smallpox was eradicated in 1980 but in 2017, Canadian scientists created a smallpox-like virus in a lab using just mail-order DNA” said UNSW Professor of Infectious Disease Epidemiology Raina MacIntyre. “In 2018, these same scientists published a step-by-step method to create a pox virus in a lab, making the threat of smallpox re-emergence even greater.”
Why is this so alarming? The only remaining stockpiles of the actual smallpox virus is heavily guarded, but with this scientific breakthrough in creating a smallpox-like virus without needing any of the remaining smallpox samples, bioterrorists wanting to create a massive viral weapon is now a reality. Additionally, we currently have an unprecedented le...
Posted by Sandy Thompson
Baby boomers are individuals born between 1945 and 1965 and currently the largest living adult generation. Based on the 2016 U.S. population ranking by age, there are approximately 74.1 million baby boomers in the United States and they have the highest incidences of hepatitis C infections.
With such a large population, combined with previous unsafe medical procedures, baby boomers are 5 times more likely to have hepatitis C than any other adult. Out of the more than three million people living with hepatitis C, three out of every four are baby boomers.
According to the CDC, most baby boomers were infected in the 1960s through the 1980s due to contact with blood from an infected person, medical equipment and procedures prior to universal precautions and infection control procedures being adopted. Additionally, baby boomers were exposed to contaminated blood supplies before widespread screening in 1992. In fact, hepatitis C was not discovered until 1989 and blood donations ...
Posted by Sandy Thompson
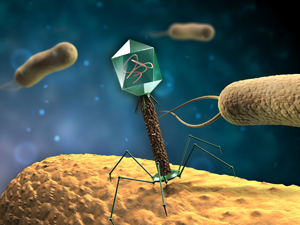
With the danger of uncontrollable bacterial infections increasing globally, a revitalized look at how bacteriophage can aid us in battling antibiotic-resistant infections is a promising alternative.
What is Bacteriophage?
Bacteriophage , or “phage” for short is a virus that infects and replicates within bacteria. There are more phage on earth than bacteria and are considered the “ Deadliest being on Planet Earth ”. Although they are lethal, they are specialized to particular bacteria in which they kill.
Phages can infect their bacteria host in two ways, known as the Lytic cycle and Lysogenic cycle. The Lytic cycle is when the phage acts like a typical virus, by hijacking the host cells and using the cell’s resources to make many new phages until eventually the cell bursts and dies. During the Lysogenic cycle, the phage inserts its DNA into the bacteria’s chromosome, where it is then replicated and spread using the bacteria’s DNA. Unde...
Posted by Kristal Roberts
The list of neurological threats related to Zika appears to be growing after a recent study concluded that the mosquito-born illness can cause a new autoimmune disease that attacks the brain and the spinal cord.
The condition is Acute Disseminated Encephalomyelitis (ADEM), and it shares certain similarities with multiple sclerosis.
The study, led by Dr. Maria Lucia Brito Ferreira at Restoration Hospital in Recife, Brazil, had 151 patients who visited the hospital from December 2014 to June 2015.
All of these patients were infected with arboviruses, which is the family of viruses that include Zika, Dengue and Chikungunya. Six of those patients had Zika and developed symptoms consistent with autoimmune disorders. These six patients suffered from fevers and rashes, both of which are Zika related symptoms. Some patients also suffered from joint pain and red eyes. Within 15 days, the patients began to experience neurological symptoms such as weakness of the extremities, headaches a...
Posted by Kristal Roberts
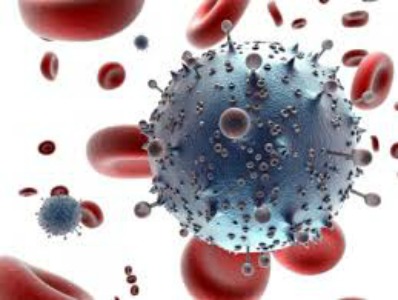
The latest global report on HIV-AIDS shows promising trends in controlling the epidemic, but some hurdles remain in improving access to life-saving treatments
A new report from UNAIDS in advance of World AIDS Day shows some impressive progress in the fight against HIV. There were 2 million new HIV infections around the world in 2014–15, the lowest since 2000, when 3.1 million people worldwide were diagnosed with HIV. Deaths from AIDS, the last stages of HIV infection, are also coming down, from a high of 2 million in the early 2000s to 1.2 million this year.
Much of that can be attributed to improved access to life-saving treatments with antiretroviral drugs (ARVs). UNAIDS says that 41% of people who are HIV positive are now being treated, nearly double the percentage in 2010. (Meanwhile, in the U.S., drugs that can prevent the transmission of HIV are proving successful, even in high-risk groups.)
While infections in sub-Saharan Africa remain high — 66% of the...
Posted by Kristal Roberts
For the past several years, the medical community has warned about the dangers of superbugs, which are potentially deadly strains of bacteria that no longer respond to antibiotics as treatment.
Well the proof is in the pudding---American scientists claims that a 30 percent decline in the efficacy of antibiotics may be responsible for some 6,000 deaths each year.
The team of scientists, lead by Professor Ramanan Laxminarayan from the Center for Disease Dynamics, Economics and Policy in Washington, D.C., also set out to discover what would happen if antibiotic resistance increased by a third (which it’s apparently on track do).
The researchers focused particularly on patients having common operations and undergoing chemotherapy treatments for cancer.
The results of the study, recently published in the Lancet, reported that this kind of antibiotic resistance could lead the U.S. to 120,000 additional resistant infections and 6300 more related deaths each year.
Laxmina...
Posted by Kristal Roberts
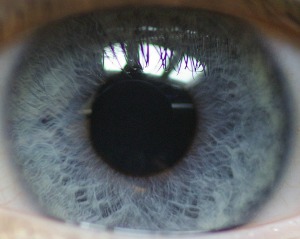
A U.S. doctor who thought he was cured of Ebola learned that wasn’t entirely true after his eye turned from blue to green and he nearly went blind.
Dr. Ian Crozier contracted the disease while treating other patients in Sierra Leone back in October 2014.
After a long, draining bout with Ebola, Crozier’s medical team at Emory University Hospital declared him cured and released him.
However, in less than two months he returned to the hospital with fading sight, pain and pressure in his left eye. To make matters worse, his eye color turned from blue to green.
What doctors found was alarming---his eyeball was filled with the Ebola virus.
It was something his medical team decided to test the eye for, but didn’t expect to find at all, The New York Times reports.
It was unexpected because after his initial treatment was completed, there were no signs of Ebola in his blood; there wasn’t a trace of the disease in his tears or even on the surfac...
Posted by Kristal Roberts
A disease that was practically non-existent in the United States took the nation by surprise last year when a reported 644 measles cases popped up. As the medical community tried to pin down the origins of this outbreak, the anti-vaccine camp (including comedian/actress Jenny McCarthy, who publicly speaks out against them, tying vaccines to autism) was identified as a possible connection to sudden surge in measles.
McCarthy, along with many others believe vaccines are dangerous and are a part of a movement that encourages parents to not vaccinate their children, which may be allowing the disease to spread more easily.
Disneyland in Orange County, California was dubbed ground zero for the most recent outbreak.
However, a recent Vox.com article traces the beginning of the recent American measles surge to an Amish missionary worker’s travels in the Philippines.
The unnamed missionary worker, dubbed patient zero, travelled from Ohio, his home state, to the Phi...
Posted by Norlyn Golez
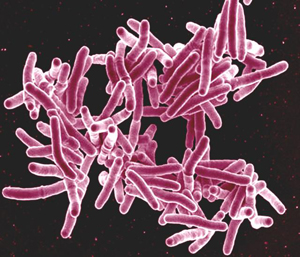
A drug-resistant strain of tuberculosis is spreading at an alarming rate, posing a risk that the world has never faced, according to Medicins Sans Frontieres/Doctors Without Borders (MSF).
TB is branded one of the most lethal diseases by the US Centers for Disease Control and Prevention (CDC). It kills around 1.3 million out of the 8 million people that it infects.
The disease is spread from one person to another when an actively infected person sneezes or coughs and the airborne bacteria are inhaled by another person. It attacks the lungs, mostly as well as other vital organs. The symptoms, include persistent coughing, weight loss, fever, night sweats, loss of appetite, and fatigue.
Standard TB can be cured, but the lack of appropriate response globally has now led to the development of a drug-resistant strain.
In fact, a journal from TheLancet.com showed that some people in South Africa have incurable TB but are still released to the community, spreading the disease.
T...
Posted by Norlyn Golez
In the case of infectious diseases, such as tuberculosis, HIV/AIDS, malaria, and other deadly diseases, detection is always the key in preventing its spread. It also helps find the most potent treatments available. The current detection methods can be prohibitively costly. However some researchers have discovered a detection method that uses common shrink wrap, which could provide an effective yet affordable detection method of these infectious diseases.
This nanotechnology method, which is the subject of a paper published in the journal Optical Materials Express, can enhance the fluorescent markers during biosensing with the use of certain metals placed onto shrink wrap.
The accessibility and affordability of shrink wrap opens develop low-cost nanostructures that have the ability to enhance fluorescence a thousand times more so even in the lowest limits. This is according to the paper’s co-author Michelle Khine, a University of California, Irvine biomedical engineering pro...
Posted by Norlyn Golez
When some people say that they prefer to recover at home rather than in the hospital to avoid getting sicker than ever, they’re probably right. That’s because your expectations of a sterile room for new patients when you first come in may not be met. There are pathogens on the surfaces of the hospital room that are not easily removed even with the use of the strongest cleaning and disinfection techniques and chemicals. They are usually pathogens that cause healthcare-associated infections (HAIs).
HAIs are actually among the largest culprits in patient mortality and morbidity. These pathogens often come from the patient’s endogenous flora, although studies have estimated that around 20% to 40% of these HAIs are actually from the healthcare personnel’s contaminated hands as they got in contact with contaminated hospital surfaces or patients. Various researches have supported that environmental contamination does aid in the easy transfer of Vancomyn-resistant En...
Posted by Norlyn Golez
The world has so far successfully controlled outbreaks of infectious diseases, but it seems like there’s no stopping the emergence of new microbes. Unfortunately, they’re not only affecting humans and animals, but the wildlife ecosystems as well.
The ecosystem has grown vulnerable to such attacks because of repeated human interventions. Large scale and accelerated production of livestock, the fast paced trade and global travel of both pet animals and domestic livestock, and our increasing disruption of ecosystems are all contributing factors. As a result, new breeds of zoonotic pathogens have emerged.
Aside from affecting human health, these new pathogens have also wreaked havoc on the social, economic, and even political aspects of various countries. Just look back to what happened in the world during the spread of Severe Acute Respiratory Syndrome (SARS), which cost the global economy around $42 billion, the Middle East Respiratory Syndrome (MERS), the avian influen...